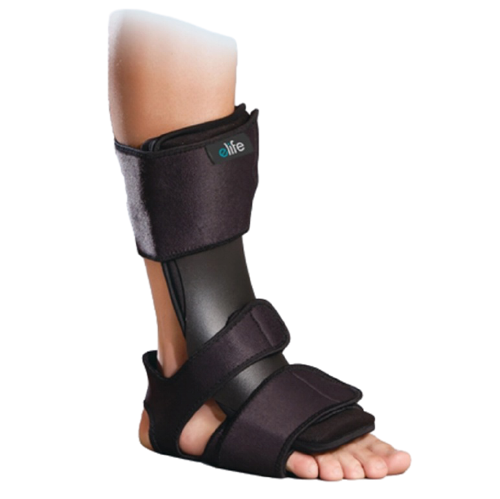
Fantastic boot! Super comfortable and love the air pump for additional ankle support. I actually put 20k steps on it the other day doing yard work and felt just fine. Highly recommended!
beautiful
USA-based company since 2005
Use this bar to show information about your cookie policy.
2 products
Showing 1 - 2 of 2 products
Fantastic boot! Super comfortable and love the air pump for additional ankle support. I actually put 20k steps on it the other day doing yard work and felt just fine. Highly recommended!
beautiful
Good stuff